"I promise not to let your child die from the disease," Cornelia Griggs, a pediatrician, reassured her neighbor Karen in New York.
In an article on NYTimes on March 19, Cornelia, a pediatric surgeon at a hospital in New York, USA, recounted a difficult conversation with Karen, a mother whose children were being treated at the hospital. Miss.
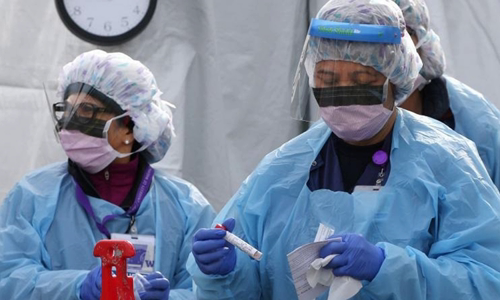
Nurses wear protective gear at the Covid-19 test area at the University of Washington medical center, Seattle Photo: AFP.
"Look into my eyes. I promise you will do your best," Cornelia said, trying to control the choking sensation in her throat. The image of the child hospitalized with countless tubes on her made her heartbreak
Two weeks ago, the Cornelia and Karen kids also ate pizza and watched cartoons, running back and forth. That was before "community separation" became a trend aimed at preventing Covid-19 from spreading in the United States.
"I can be somewhat reassuring about the promise to Karen, because statistics show that children don't seem to be much at risk of dying from Covid-19. But I can't make the same promise to many others," Cornelia writes.
A few days later, this female doctor received a message from her best friend. She has asthma. "I told you this just because someone needs to share it," the text said.
The friend said that if she was ill and had a bad prognosis, Cornelia recorded the voice of her 4-year-old daughter Josie for her to hear. "I think it will save my life," she said.
At Cornelia Hospital, one of New York's largest medical centers, the number of nCoV infections continues to rise, forcing hospital leaders to reallocate as many medical staff as possible to the room. emergency room, isolation room and intensive care room.
Cornelia said that this is a scenario that everyone needs to join hands to cope, but predicts the situation may worsen in the near future.
"The sky is falling. I'm not afraid to say this. In a few weeks, I might be considered a bewildering propagator, but that's okay. I'm even happier if I have a feeling." her is wrong, "she said.
Cornelia, a specialist surgeon and emergency resuscitation specialist, asserted that she was not the one to give unfounded information. She has spent most of her training to participate in trauma surgeries in emergency rooms and internships in intensive care units at Harvard University Hospital and currently has the last 4 months of surgery training. Pediatrics in New York City.
"My job sometimes requires waking up in the middle of the night to run to a pediatric hospital and saving many babies' lives with ECMO, an out-of-body circulatory technique used when a child suffers from respiratory failure despite using a machine. breathe, "she described.
The late-stage Covid-19 adaptation drills are also part of Cornelia's work. After 9 years in the medical profession, panic no longer exists in her dictionary. But this time was completely different.

Medical personnel tie the mask at Roper St Hospital Photo: AP.
"We are experiencing a global public health crisis, with unprecedented speed and scale. The gaps in the health and financial systems have been exposed in this pandemic. How does this translate, the lives of all of us will forever change, "she said.
At the frontline anti-Covid-19 health facilities, patients lined up outside the clinic and emergency room to wait for answers, but the health system's resources were limited. Only after March 13 can health agencies in New York be able to conduct nCoV testing more easily, but it is still very limited.
Right next to Cornelia's office in the hospital, a lab is being transformed into a laboratory in the hope of being able to perform 1,000 tests a day. But testing guidelines and criteria change day by day, putting the US health system in uncertainty. Hospital leaders work tirelessly, but doctors in the departments are pessimistic about their ability to meet the surging treatment needs of nCoV-infected patients.
"Earlier this week, the pediatric hospital where I worked was about to run out of gloves and other protective gear. This is bad for health workers and patients at high risk of infection. In addition to protective equipment , many other supplies of medical supplies are also exhausted, "Cornelia revealed.
New York City Hospital has 4,000 patient beds, but only is equipped with 500 permanent ventilators and 250 backup machines. If the number of infections is increasing as fast as in Italy, New York will soon run out of breathing apparatus.
"Viral treatment" methods are still in the early stages of testing and are difficult to get approved in the short term. "I repeat, the sky is falling," the female doctor said.
Cornelia said that she issued this warning not to make people panic, but to call for action together. "We need more medical supplies right now, especially gloves, masks, goggles and ventilators. We need a team of technology engineers to make and test systems that can. "Improving breathing machines to increase patient support. We need laboratories to concentrate all resources to quickly research vaccines and antiviral methods against Covid-19."
She also said that American hospitals need to quickly adjust existing methods to cope with nCOV. Doctors across the globe need to share information, guidance and strategies through social networks, because traditional information channels are too slow.
The female doctor urged everyone to join hands to minimize the number of new cases by staying indoors. "Like everyone, I was sometimes terrified when I thought of the worst Covid-19 scenarios possible. But negative thinking doesn't help. Instead of panicking in solitude. , we need to work together, "she wrote.
"We, who are in contact with the Covid-19 patients every day, desperately need you, need your mind, need creative solutions and need your voice to fight for us. It may be exhausting when trying to provide emergency services to every patient who steps into the hospital door, but if everyone is involved, I promise not to panic. to save lives for everyone. Therefore, everyone please do the same for us. "



 PoeZarniKyaw
PoeZarniKyaw







